
Temporary COVID-19 Relief for Section 125 Plans
On Feb. 18, 2021, the IRS released Notice 2021-15 to clarify special rules for Section 125 plans, health flexible spending arrangements (FSAs) and dependent care assistance programs (DCAPs).
Special Rules for Health FSAs and DCAPs
The Notice is intended to clarify the application of special rules for health FSAs and DCAPs under the Consolidated Appropriations Act, 2021 (CAA). The CAA provides flexibility for carryovers of unused amounts, extends the time period for incurring claims, allows post-termination reimbursements from health FSAs and provides special rules for dependents who “age out” of DCAP coverage during the COVID-19 public health emergency. The Notice provides details and examples regarding these rules.
Section 125 Mid-year Election Changes
The Notice’s relief for mid-year Section 125 plan elections for plan years ending in 2021 is similar to prior guidance for 2020. Section 125 plans may allow employees to make or revoke election changes in certain circumstances.
The Notice clarifies that employers can decide how long to allow mid-year election changes with no change in status during the plan year and can limit the number of election changes during the plan year that are not associated with a change in status.
Over-the-Counter Drugs
The Notice also provides relief with respect to plan amendments expanding reimbursable expenses for health FSAs and HRAs to include over-the-counter drugs and menstrual care products. Amendments to these plans must normally be made on a prospective basis, but these amendments may allow these reimbursements beginning on or after Jan. 1, 2020.

COBRA Subsidy Provisions of the American Rescue Plan Act
The American Rescue Plan Act (ARPA), signed into law March 11, 2021, provides a 100% subsidy of premiums for employer-sponsored group health insurance continued under the Consolidated Omnibus Budget Reconciliation Act of 1986 (COBRA) and similar state continuation of coverage (mini-COBRA) programs.
ARPA subsidies cover the full cost of COBRA or mini-COBRA premiums from April 1, 2021, through Sept. 30, 2021, for employees (and their qualifying family members), if the employee lost or loses group health insurance due to an involuntary job loss or reduction in work hours. The subsidy applies to people who are still within their original COBRA or mini-COBRA coverage period, for the length of that coverage period, even if they declined or dropped COBRA or mini-COBRA coverage earlier.
The subsidy does not apply to:
- Individuals whose job loss was voluntary or the result of gross misconduct; or
- Individuals who are eligible for another group health plan or Medicare.
Overview
COBRA requires group health plans to allow covered employees and their dependents to continue their group health plan coverage when it would be lost due to specific events, such as a termination of employment or reduction in working hours. Individuals are usually allowed to continue their COBRA coverage for 18 months, although some similar state mini-COBRA laws mandate a longer coverage period.
Under COBRA, group health plans may require those covered to pay 102% of the premium for their continuing health insurance, leading many eligible individuals to decline coverage. The ARPA subsidy covers the full cost of COBRA or mini-COBRA premiums from April 1 - Sept. 30, 2021, for "assistance-eligible individuals."
Covered Plans
The COBRA subsidy in the ARPA applies to group health plans subject to federal COBRA or to a state mini-COBRA program. Plans subject to federal COBRA are plans maintained by employers with 20 or more employees on more than 50% of the business days in the previous calendar year. Small-employer plans, small governmental plans and church plans are not subject to federal COBRA, but may be subject to a state mini-COBRA law and therefore be covered by the ARPA's COBRA subsidy provisions.
Health flexible spending arrangements under Section 125 cafeteria plans are not covered by the ARPA COBRA subsidy.
Eligible Individuals
Individuals are eligible for the COBRA subsidy if they:
- Are a qualified beneficiary of the group health plan; and
- Are eligible for COBRA or mini-COBRA continuation coverage because of the covered employee's involuntary termination (unrelated to gross misconduct) or reduction in hours of employment.
The subsidy is not available for people who voluntarily left their job. It is also unavailable for people who are eligible for Medicare or another group health plan, not including:
- A plan covering only excepted benefits;
- A qualified small employer health reimbursement arrangement; or
- A flexible spending arrangement.
Furthermore, individuals receiving a COBRA subsidy who become eligible for a group health plan or Medicare must inform the health plan for which they are receiving the subsidy of that fact, or face a penalty. The premium subsidy is not counted as gross income.
Extended Election Period
The ARPA allows individuals to elect subsidized COBRA if they:
Become eligible for COBRA or mini-COBRA due to involuntary job termination (not caused by gross misconduct) or reduction in hours between April 1 and Sept. 30, 2021;
- Previously declined COBRA or mini-COBRA after becoming eligible due to involuntary job termination (not caused by gross misconduct) or reduction in hours, but would still be within their COBRA or mini-COBRA coverage period had they elected the coverage at that point; or
- Previously elected COBRA or mini-COBRA but discontinued the coverage before April 1, 2021.
- The election period for subsidized COBRA under ARPA begins on April 1, 2021, and runs until 60 days after the date individuals receive notice from the health plan of the availability of the COBRA subsidy.
Duration of Coverage
COBRA and mini-COBRA coverage under the ARPA election extension starts with the first period of coverage beginning on or after April 1, 2021, and continues through the end of the individual's COBRA or mini-COBRA coverage period. The individual's COBRA or mini-COBRA coverage period is the period that would have applied had the individual elected the continuation coverage when first eligible following the initial qualifying event. For individuals who previously elected COBRA or mini-COBRA, discontinued it, and are now using the ARPA extended election period to obtain COBRA, the COBRA coverage period is calculated as if they had not dropped the coverage.
Switching Coverage
The ARPA contains a provision that-at the employer's option-allows individuals eligible for the COBRA subsidy and enrolled in the employer's group health plan to change to different health coverage also offered by the employer. The new coverage cannot have a higher premium than the individual's previous coverage, and it must be offered to similarly situated active employees. The option does not apply to plans that provide only excepted benefits, to qualified small employer health reimbursement arrangements or to health flexible spending arrangements.
The change must be elected within 90 days of the employee receiving notice of the option.
Notice Requirements
The ARPA imposes new COBRA notice requirements on health plans.
General Notice
Plan administrators must provide notification of COBRA benefits under ARPA. The notice must be written in clear and understandable language, and it must inform recipients of the availability of ARPA premium assistance and the option under the ARPA to enroll in different coverage (if the employer permits the option).
The notice must be provided to individuals who become eligible for COBRA or mini-COBRA during the period of April 1 - Sept. 30, 2021. In addition, it must be provided by May 31, 2021, to people who have already elected COBRA coverage, and to people subject to the ARPA election extension-that is, people eligible for the subsidy who declined or discontinued COBRA or mini-COBRA before April 1, 2021.
The notification may be included in an amendment to a plan's existing notices or be given in a separate notice, but it must contain the following information:
- The forms necessary for establishing eligibility for premium assistance
- The name, address and telephone number necessary to contact the plan administrator and any other person maintaining relevant information in connection with premium assistance
- A description of the extended election period under the ARPA
- A description of the obligation of qualified beneficiaries to notify the plan if they become eligible for another group health plan or Medicare, and the penalty for failure to do so
- A prominently displayed description of the right to a subsidized premium and any conditions on entitlement to the subsidized premium
- A description of the option of the right to enroll in different coverage (if the employer permits this option)
The DOL is charged with issuing a model general notice by April 10, 2021, for plans to use to meet the general notice requirement.
Notice of Expiration of Subsidy
Plans must also provide individuals eligible for the ARPA subsidy with notice of its expiration. The notice must be written in clear and understandable language, and inform recipients that:
- The premium assistance will expire soon, prominently identifying the expiration date; and
- The individual may be eligible for coverage without premium assistance through COBRA continuation or a group health plan.
Plans are not required to issue an expiration notice to individuals whose subsidy is expiring because they became eligible for other group health plan coverage or Medicare.
The notice must be provided during the 45 - 15-day period before the individual's subsidy expires. The DOL must issue model expiration notices by April 25, 2021.
Tax Credit
The ARPA COBRA subsidy is funded through a tax credit to employers whose plans are subject to federal COBRA or are self-insured, to the plan for multiemployer plans, and to the insurer for other plans. The credit is taken against payroll taxes. It can be advanced (according to forms and instructions to be provided by federal agencies) and is fully refundable. The credits will be provided each quarter in an amount equal to the premiums not paid by assistance-eligible individuals.

Top 10 Workplace Discrimination Claims
In the 2020 fiscal year, the Equal Employment Opportunity Commission (EEOC) resolved more than 70,804 charges of workplace discrimination. Discrimination lawsuits can be very time-consuming and expensive for employers, and can result in a loss of employee morale or reputation within the community.
Top Causes of Discrimination
According to the EEOC, the following are the top 10 reasons for workplace discrimination claims in fiscal year 2020:
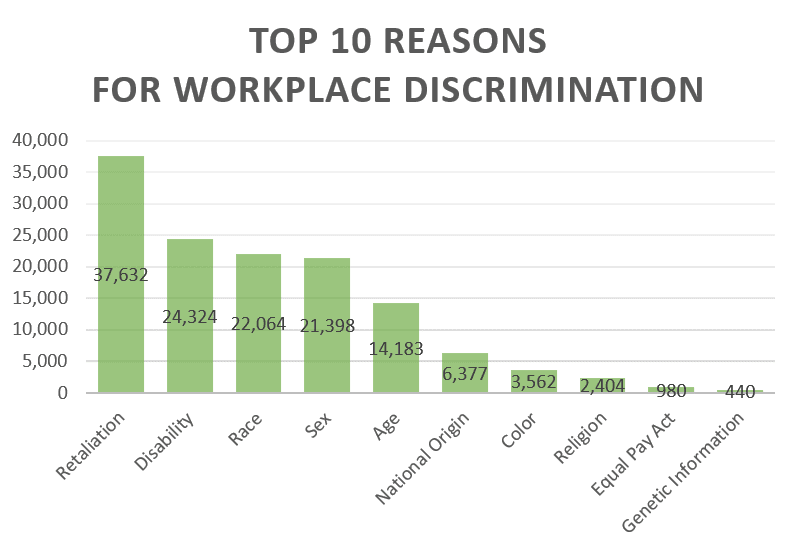
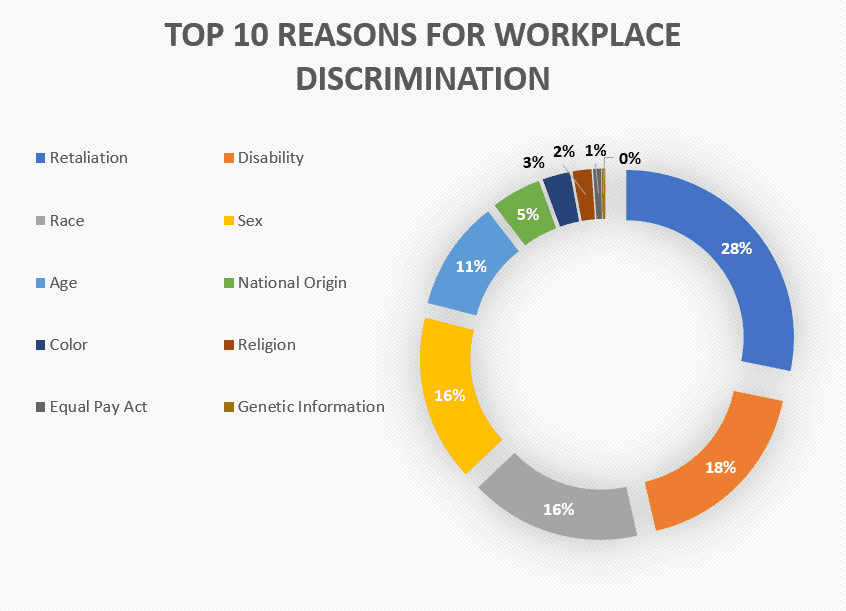
These percentages add up to more than 100% because some lawsuits were filed alleging multiple reasons for discrimination.
Steps for Employers to Protect Themselves From Discrimination Claims
Employers should consider the following steps to protect themselves from retaliation and other discrimination claims:
- Audit their practices to uncover any problematic situations.
- Create a clear anti-retaliation policy that includes specific examples of what management can and cannot do when disciplining or terminating employees.
- Provide training to management and employees on anti-retaliation and other discrimination policies.
- Implement a user-friendly internal complaint procedure for employees.
- Uphold a standard of workplace civility, which can reduce retaliatory behaviors.
- For more information and for tips on how to protect your business, reach out today.
- Benefits Education for Young Employees
Employee benefits aren’t always simple. In fact, for many young employees, they’re downright confusing. Look at basic health insurance term knowledge, for example. Only 7% of individuals can define terms like premium, deductible and coinsurance, according to UnitedHealthcare. Here are five ways you can start informing young employees about their benefits right away:
1. Start with benefits 101— Start educating with benefits 101 initiatives, assuming employees have no base knowledge. Resources in this area cover insurance basics, such as common terms, group health coverage ins and outs, and enrollment period restrictions.
2. Explain what’s in it for them— At the core of any transactional conversation is the question of “What’s in it for me?” Employees, especially younger ones, will undoubtedly want to understand why it’s worth it to learn insurance basics.
3. Vary the messaging— Use several formats to help reinforce benefits literacy among employees and capture more attention. Examples include email announcements, PowerPoints, videos, mail-home flyers, posters and comprehensive packets.
4. Don’t stop educating— Benefits literacy isn’t something achieved overnight. Rather, it should begin immediately and continue year-round.
5. Be there for questions— Have a dedicated person on the HR team help answer benefits-related questions. This individual should be available to respond to emails as well as attend in-person or virtual meetings.
You have a responsibility to educate your employees about their benefits. Young employees can’t be expected to understand their benefits nor make wise health care choices if they don’t understand benefits basics. Reach out for sample employee education materials.

How to Conduct a Job Interview
The most important tasks in conducting a job interview are preparing questions and evaluating candidate answers. However, there are other key items you can attend to that will ensure a successful job interview. Learn the action steps you need to know by watching the video below.
The content herein is provided for general information purposes only, and does not constitute legal, tax, or other advice or opinions on any matters. This information has been taken from sources which we believe to be reliable, but there is no guarantee as to its accuracy.
Copyright © 2020 HR 360, Inc. All rights reserved.
