
Typical service transactions are straight forward. When you walk into your frequented barber shop or hair salon, you should have a pretty good idea of what the bill will be when the service is complete. You will receive the service and pay the bill before heading out the door. All done! This familiar process translates to an oil change, car wash, pet grooming, and many other services we consume on a regular basis. Where we do not see this transaction sequence, is when purchasing healthcare services.

The Healthcare Transaction Process
It is important that you, as a healthcare consumer, feel confident in the accuracy of the payment you send to your provider after a healthcare visit. Healthcare reimbursement is a multi-step, lengthy and complicated process that could go a little something like this;
1. A patient visits their healthcare provider for a particular service and checks in, presents their ID card and pays a copay fee if applicable.
2. The patient receives care from their healthcare provider, who enters notes into an electronic file throughout the visit. These notes will later be used to create codes that the insurance carrier pays by.
3. The patient’s visit is concluded and the patient leaves with no immediate bill or charge aside from a possible copay.
4. The codes interpreted from your healthcare provider’s notes will be sent in an electronic data file to your insurance carrier, which will likely be automatically adjudicated and paid by the carrier.
5. The patient will receive their explanation of benefits (EOB) from the insurance carrier and an invoice from the doctor’s office if additional payment is needed.

Know the Cost of Your Healthcare Before Receiving It.
If a possible unknown medical bill in the mail from your healthcare visit stirs up more fear in you than the effects of untreated injury and illness, this article is for you. The Healthcare Transparency Rule, effective January 1, 2021, brings patients closer to knowing what care will cost before a visit to the doctor even happens. Read more >>>

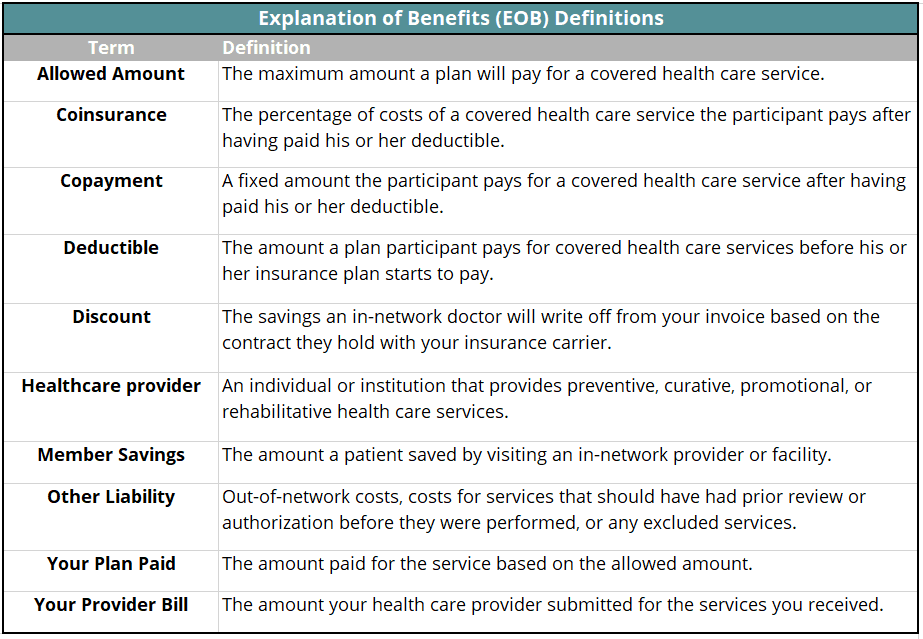
The Explanation of Benefits
An explanation of benefits, or EOB, is a summary of your insurance benefits that have been applied to your medical claim. It is important to note that an explanation of benefits is NOT a final invoice and should not be treated as such. A crucial area of the patient’s EOB that should be examined is under ‘Member’s Responsibility’. The amount listed under ‘Member’s Responsibility’ should exactly match the amount due in the invoice from your doctor’s office. If the EOB and invoice amounts do not match, it is time to give your company’s Benefit Broker a call for assistance in resolving the claim discrepancy.
EOBs should be filed and stored away for future reference.
Making a Payment:
When a claim has been finalized, either the insurance company will cover the invoice in full, or an outstanding payment will be requested of the patient. When a patient receives the invoice from their doctor’s office and has confirmed that the amount due matches the EOB, a few pieces of information are needed to complete the payment.
1. Date of healthcare service(s) provided.
2. Patient ID number and billing number.
3. Total amount owed by patient, not covered by insurance carrier, to service provider.
Keep in mind that if you have a high-deductible or other qualifying plan, your HSA is an acceptable method of payment.

What is a Health Savings Account?
A health savings account, or HSA account, is a savings account where you can deposit money on a pre-tax basis to pay for qualified medical expenses. The list of qualified medical expenses is huge... Read more >>>

Asking for Help
When in doubt, contact your employer’s Benefits Broker for assistance resolving billing and claims discrepancies, help understanding your explanation of benefits or other insurance and billing related questions. For Forsite Benefits' clients, rely on our Forsite Assist team for benefit guidance. If you find your explanation of benefits does not match the doctor’s invoice, reach out to your doctor’s office for an itemized list of services and invoice coding to ensure coding is correct before finalizing a payment.
Did you enjoy this educational read?
Check out our library of Nav Series newsletter topics and remember to subscribe to our employee healthcare education and receive a new healthcare topic each month to your inbox!
